Very low bone density is known as osteoporosis. It can predispose you to fractures and impact many areas of your life. Let us help you.
Introduction
Our bones are made up of a hard-living material that builds up strength during our youth, reaching its peak in our 4th decade of life (the 30s). One of the important components of bone is calcium, and this balance of storing calcium and removing calcium in bones is tightly regulated in the human body.
As we grow older, our bones progressively start to get weaker, losing strength. This is due to both a loss in the amount and quality of bone. Bone has a very intricate structure, with a solid outer layer known as the cortex, and a net-like inner portion known as trabeculae.
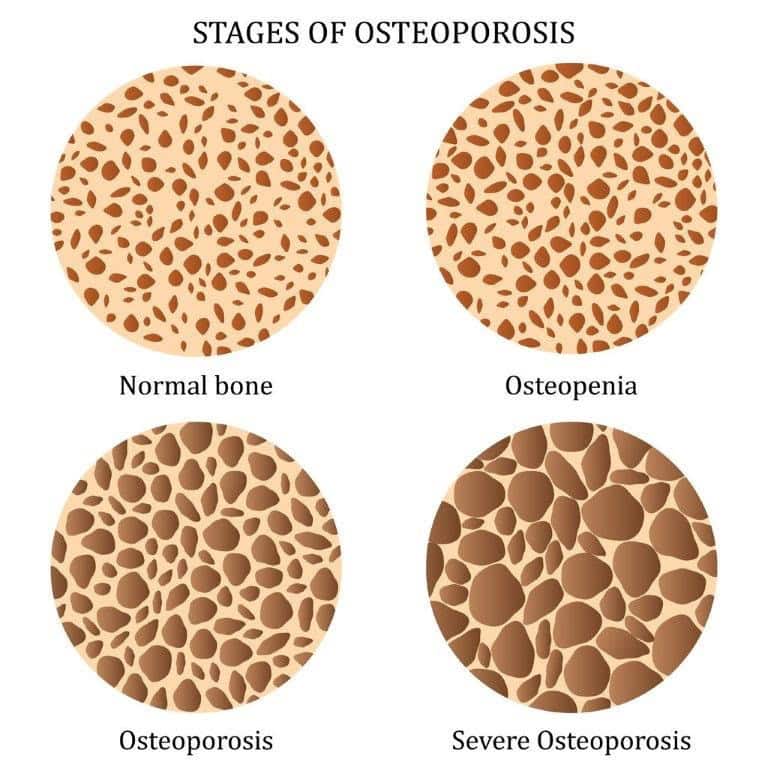
The loss in bone is most apparent in the trabeculae. As bone density decreases, the ‘holes’ in the net-like trabeculae get larger. This loss is permanent, and there is currently no way to replace lost trabeculae.
In general, ladies lose bone at a greater rate than men. This difference is more apparent after menopause. This loss of bone density can be measured, and once it reaches a critical stage, it is known as osteoporosis.
What are the problems with low bone density?
Low bone density predisposes a person to fractures. The lower the bone density the higher this risk is. Depending on the affected body part, this can have further repercussions on a patient’s life and livelihood.
Commonly affected areas are the wrists, the hips and the spine. In the wrists, low bone density can predispose to distal radius fractures, which are fractures affecting the wrist bones. These commonly occur due to falls in the elderly. Once broken, the wrists are usually deformed, and wrist and hand function is usually affected adversely. This may make it hard for the patient to feed and clothe themselves.
The hips are another commonly affected area, with hip fractures in the elderly seen as an epidemic across the world. Hip fractures usually render a patient immobile and bedbound. This immobility can lead to pressure sores, infections of the urinary tract and lungs, and blood clot formation in the legs and lungs. In un-operated hip fracture patients, the 1-year mortality has been reported to be as high as 25%.
In the spine, low bone density often results in compression fractures, where the spinal bones get compressed and flattened. Not only does this cause severe pain, but over time, patients find themselves hunching more. In severe cases, the patient can no longer stand upright.
While these areas are commonly affected, every bone in the body is weakened by osteoporosis, fractures can therefore affect many other areas in the body. It is therefore crucial that patients with low bone density be assessed and treated before a fracture happens.
Why Do I Have Low Bone Density?
In most patients, the reason for low bone density is not known. That is not to say that it happens without any reason. Rather, there are many possible risk factors, with no factor thought to be more important than others.
Possible risk factors include:
Vitamin D deficiency is being recognized as one of the more important factors in low bone density. Vitamin D is a naturally occurring substance that is formed in our bodies on exposure to sunlight. It is important in the absorption of calcium from food, and its retention in our bodies as bones.
How Can We Diagnose Low Bone Density?
Usually, patients with low bone density present after a fracture. This is usually a low energy fracture, in which the injury seems like it would not cause a severe injury. This can range from breaking a toe while accidentally kicking an object, to any of the previously mentioned fractures.
Once your doctor suspects that you have low bone density, he/she will refer you for a special scan known as a dual energy x-ray absorptiometry or DEXA scan, which will allow the assessment of bone density in the body. This is usually performed on the spine and the hip, two commonly affected areas.
He/she may also order some blood tests to check the calcium and vitamin D levels in the body. Based on this information, the doctor will be able to diagnose low bone density and offer you treatment for your problem.
What are the Available Treatments for Osteoporosis?
Currently, there is no way to completely reverse osteoporosis. We can slow down the rate of bone loss, and even reverse the loss in bone density, but medical science is currently unable to recreate the net-like trabeculae, which is important for the strength of bones.
Despite these challenges, there are some good options available:
In addition to these methods, patients currently being treated for osteoporosis are recommended to undergo yearly or twice-yearly screening of their bone density, in order to monitor progress of the disease and correct any nutritional imbalances that exist.
9898 3595 (Call & WhatsApp)
[email protected] (Email)
Lorem ipsum dolor sit amet consectetur adipiscing elit ut arcu a dignissim suscipit non ac eget tellus in nisl mauris nec.
